What are painful vertebral compression fractures?
50% of women and 25% of men in the USA will develop an osteoporotic compression fracture in their lifetime.
A vertebral compression fracture (VCF) is a compression deformity caused by stress (often as trivial as sneezing) applied to a vertebral bone weakened by osteoporosis, malignancy, or metabolic disorder. Weight-bearing vertebral bodies in the low thoracic and lumbar spine are most commonly involved, but fractures can occur in any part of the spine, including the sacrum. A VCF may lead to deterioration of the quality of life and decline in health due to severe pain and decreased mobility.
What are the symptoms of painful vertebral compression fractures?
Vertebral compression fractures typically present with the following symptoms:
- Sudden onset of back pain
- Back pain localizes to the midline
- Pain radiates in a band-like manner around the torso
- Pain is unresponsive to medical therapy
- Standing or walking worsens the pain
- Lying on the back makes the pain better
- Pain is associated with limited spinal mobility
What are the causes of vertebral compression fractures?
Vertebral compression fractures occur as a result of a weakening of the vertebral bones. Thus, most spinal compression fractures are found in elderly patients suffering from osteoporosis. A VCF can also be associated with primary or metastatic cancers involving the spine. These fractures can also result from a fall or other trauma. However, in patients with severe osteoporosis, even sneezing or bending to pick something up off the floor may lead to vertebral compression.
Who is at risk for painful vertebral compression fractures?
The following are the risk factors for developing vertebral compression fractures:
- Elderly patients
- Patients with osteoporosis
- Patients with a previous history of vertebral compression fractures
- Female gender
- Caucasian ethnicity
- Patients exposed to steroid therapy
- Sedentary patients
- Smokers
- Patients with calcium/vitamin D deficiency
- Patients with cancer
What are the consequences of untreated painful vertebral compression fractures?
Vertebral compression fractures typically begin with the sudden onset of sharp, debilitating back pain. Left untreated, the fractured vertebral body will likely continue to collapse with the onset of chronic pain, kyphosis (hump deformity), loss of vertebral column height, and a general decline in health, the progression is known as a downward spiral when all functions gradually deteriorate due to pain-induced immobility.
Who is a candidate for the treatment of painful vertebral compression fractures?
Patients with new or recent onset of back pain should be evaluated for causes of pain, including diagnosis of vertebral compression fractures. The diagnosis is based on history, physical exam, and findings of the radiographic imaging, such as an X-ray, CT scan, or MRI.
What is the treatment of painful vertebral compression fractures?
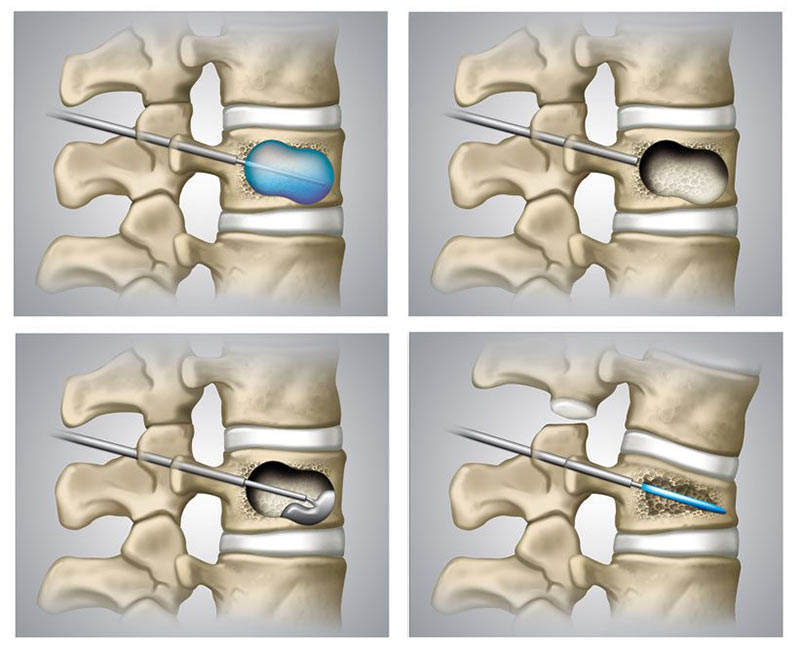
Vertebral compression fractures are treated with vertebral body augmentation when internal fixation of the affected bone is achieved by intraosseous (inside the bone) installation of a hardened cement or metal scaffolding using techniques such as vertebroplasty, kyphoplasty, or Spine Jack.
These procedures are usually performed under moderate sedation. Using fluoroscopy as image guidance, a fractured vertebral body is identified while the patient is on the procedure table. Via a 2 mm nick in the skin on the back, hollow needles are guided into the fractured vertebrae under real-time fluoroscopic guidance. Depending on the technique, a fracture decompression may be implemented first to restore some of the lost vertebral body height, followed by the installation of an orthopedic cement or metal scaffold inside the fractured bone. The procedure takes about 1 hour.
What is the recovery after endovascular treatment of painful vertebral compression fractures?
Following a brief post-operative recovery, patients go home and resume normal activities on the same day. Pain relief is expected immediately after the procedure, with some residual soreness from the incisions lingering for 2-3 days.
Treatment is available in Brooklyn, NY
If you are experiencing new or recent back pain, please contact Dr. Sergei Sobolevsky to schedule a consultation. A detailed evaluation of the back pain is necessary to make a precise diagnosis and delineate a treatment strategy.
Call the Downtown Vein & Vascular Center at 718-787-5559 to speak with a representative or schedule a consultation online today! You can also read more about fibroid, vein, and artery treatment.
Downtown Vein Treatment Center
480 Court Street, Ste 101
Brooklyn, NY 11231
(718) 787-5559


